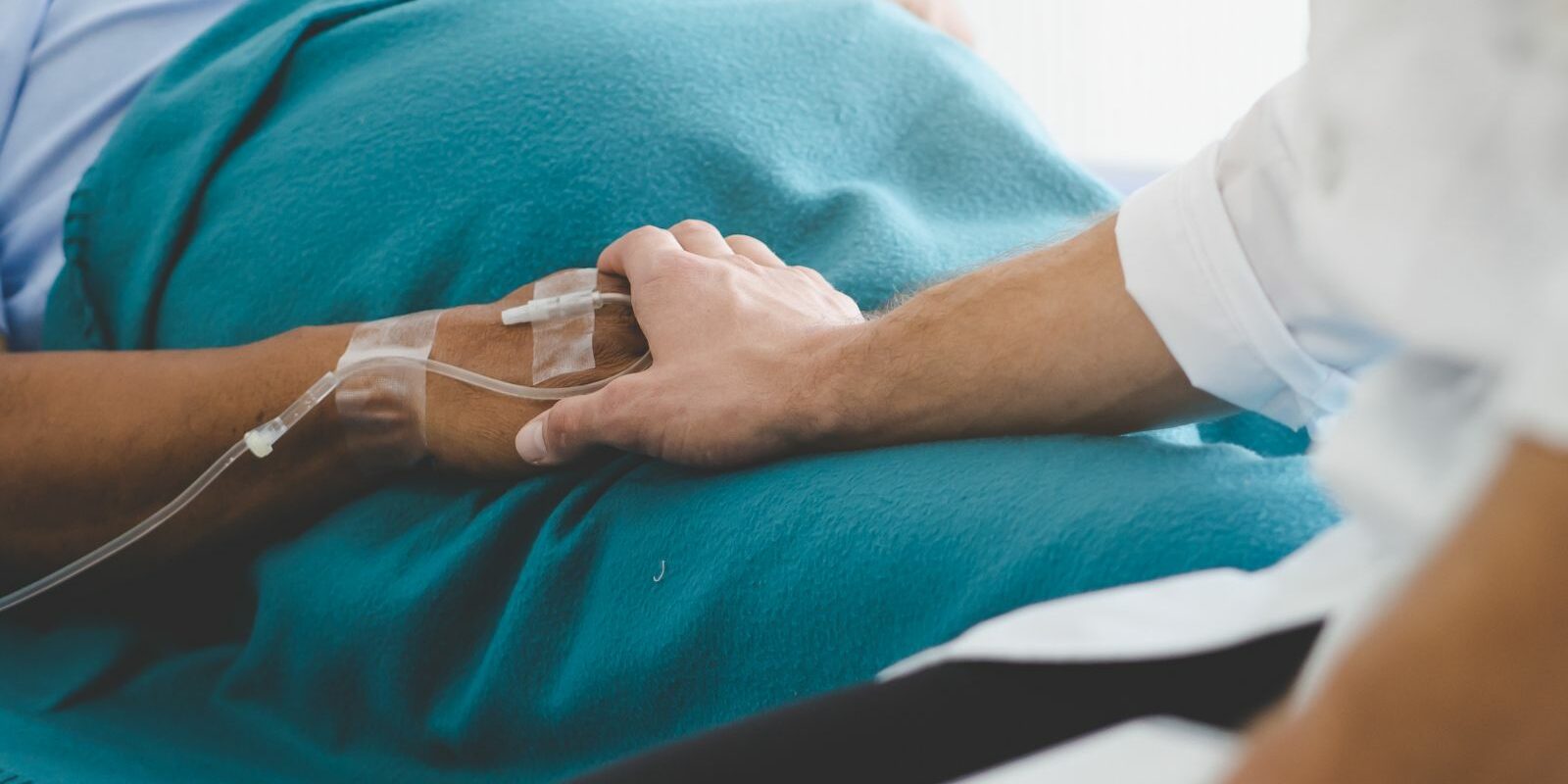
Deficiency risk after BPD
Deficiency risk after BPD
Sustainable weight loss, but increased micronutrient deficiency risk after a BPD
The BPD, short for Biliopancreatic Diversion, is a complex bariatric operation with good long-term results regarding weight loss. With the increased complexity of this procedure, the risk of negative effects may also increase. This study addressed the positive and negative results of the procedure, including the nutritional deficiency risk after a BPD in 64 morbidly obese patients who were followed up for 3 years after surgery.
Huge health benefits after BPD
The BDP proved to be an effective method for losing weight: the excess weight loss increased from 29.3% at 6 months postoperatively to 61.5% at 3 years after surgery. Besides the sustainable weight loss, BDP significantly reduced several comorbidities. Before surgery, 8 patients had diabetes and 6 patients had hyperlipedemia. 9 months after BPD, blood levels indicating both comorbidities were back to normal for all patients. Furthermore after 9 months, sleep apnea, occuring for 3 patients before surgery, was improved, and blood pressure went back to normal levels for 83,3% of the patients.
Increased prevalence of micronutrient deficiencies
Despite the advise for al pagients to use a multivitamin, the prevalence of deficiencies for ferritin, vitamin A, D and B12, zinc and copper increased significantly over the 3-year period. Only folic acid deficiency, which was found in half of the patients before BDP, decreased to 5.5% after 3 years. To reduce the risk of nutritional deficiencies, proper monitoring of the nutritional status is needed. Furthermore, advice for long-term supplementation is essential after BDP to prevent severe clinical and biochemical deficiencies.
For more information about the article, get in touch with us by clicking the button below.
Reference:
De Luis et al. (2008) Clinical results and nutritional consequences of biliopancreatic diversion: three years of follow-up. Annals of Nutrition and Metabolism, 53: 234-239.