Patient adherence to multivitamin supplementation after bariatric surgery
Patient adherence to multivitamin supplementation after bariatric surgery
Review of factors that influence adherence
Bariatric surgery patients face a lifelong road of supplementation after surgery. Although multivitamins are essential at avoiding nutritional deficiencies, too often patients discontinue treatment. How come? Don’t they know the importance of supplementation?
Well… it’s not that simple. In fact, there are a variety of factors that can influence adherence in bariatric patients. A narrative review by Smelt et al. identifies the main factors that can influence how well patients follow post bariatric surgery supplementation.
Why do bariatric patients need supplements?
Following bariatric surgery, patients undergo drastic physical changes that can cause:
- reduced food intake
- changes in eating patterns
- food intolerances
- gastrointestinal symptoms
- malabsorption
All these changes, coupled with an unbalanced diet, can cause micro and macro nutrient deficiencies.
Adherence after 4 years
The literature indicates that deficiencies are rampant on patients who do not comply with standardized nutritional care following bariatric surgery. Over a 3-year period, specific nutritional deficits occurred more frequently in patients who did not adhere to long-term multivitamin supplementation compared to those who were compliant.
Deficiencies 3 years after Bariatric Surgery
| Non-adherence patient group (n=32) | Adherence patient group (n=66) |
|---|---|
| 4.2±1.9 deficiencies (P<0.01) | 2.9±2.0 deficiencies (P<0.01) |
| 44% subjects ≥5 deficiencies | 15% subjects ≥5 deficiencies |
It’s worth noting that the number of vitamin deficiencies was found to be correlated with the time elapsed since the patient last visited their healthcare professional. Time from the last visit was significantly higher in non-adherence patients with a gap of 22 months between adherence (11.9±1.5 months) and non-adherence patients (34.1±8.3 months).
Adherence influencers in Bariatric Patients
Smelt et al. categorizes the factors that influence compliance into 5 groups:
- Patient-related: demographic and socioeconomic factors (age, sex, employment, postoperative complications and postoperative complaints and eating behaviour).
- Therapy-related: the multivitamin regimen, side-effects, pill size, disintegration properties, and forgetfulness.
- Physiological and economic factors: cost and perceived value of the multivitamin regimen.
- Healthcare-related: frequency of medical visits
- Bariatric surgery-related: postoperative complications/complaints such as vomiting, food intolerance, nausea, bloating, diarrhea, gastroesophageal reflux, marginal ulceration, intestinal obstruction, and stomal outlet stenosis.
Understanding the reasons that influence bariatric patients to stop taking supplements is crucial at minimizing deficiencies and the health complications that arise as a consequence. Unfortunately, poor adherence is a real issue among bariatric patients. In fact, the literature shows a significant decrease in compliance to multivitamin supplements 4 years after bariatric surgery.
Percentage of patients who take supplements 1 vs 4 years after surgery
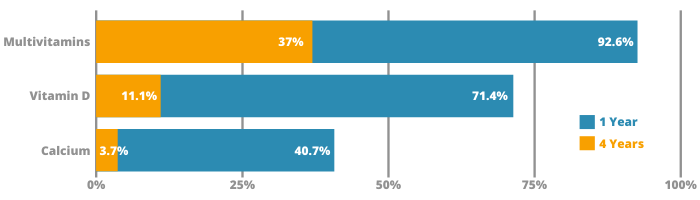
The authors expanded the scope of the review to other patient groups in order to have a wider understanding of factors that affect compliance.
Additional adherence influencers in Other Patient Groups
The narrative review introduces additional adherence influencers in patients with chronic diseases which have not yet been studied in bariatric patients.
- Patient-related: education and income.
- Therapy-related: duration of treatment and dose frequency.
- Physiological and economic factors: lack of knowledge about medication, feeling unsusceptible to the illness, negative attitude towards medical therapy.
- Healthcare-related: unsatisfaction with clinical visits, inadequate follow up or discharge planning, and poor patient-doctor relationship.
These additional factors can prove useful in increasing long-term adherence for bariatric patients. Smelt et al. prescribe patient-centered education which emphasizes the need for bariatric teams as a crucial step in increasing long-term adherence.
Would you like to learn more about this narrative review? Contact us by clicking on the button below:
Source: Smelt, H., Pouwels, S., Smulders, J., & Hazebroek, E. (2020). Patient adherence to multivitamin supplementation after bariatric surgery: A narrative review. Journal of Nutritional Science, 9, E46. doi:10.1017/jns.2020.41





